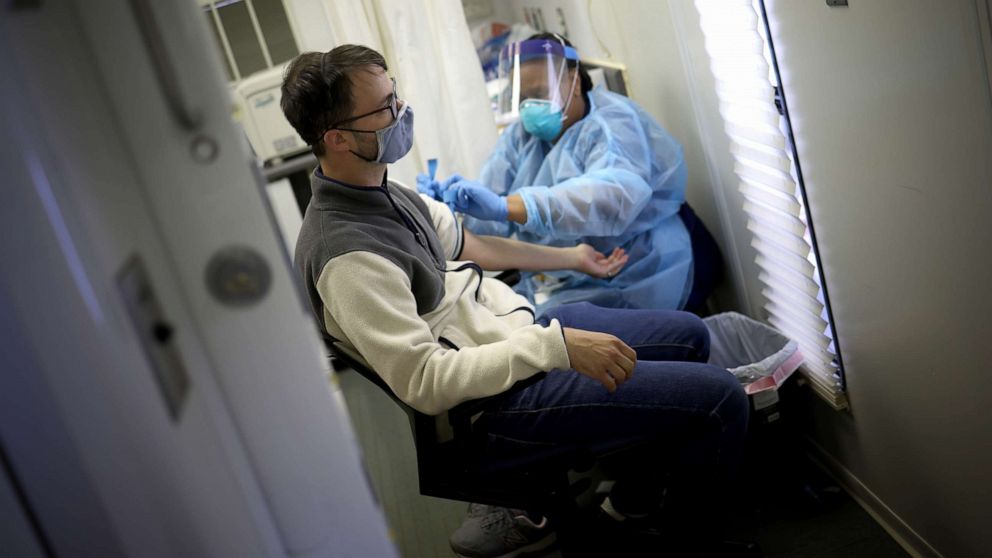
As the world faces the COVID-19 pandemic, a new study suggests that antibodies, proteins produced by the immune system that can provide protection against reinfection, may disappear in just two months after infection in certain people who have recovered from the virus.
The study was conducted in China and published in Nature Medicine.
Specifically, the study authors found that people with COVID-19 who never develop symptoms can see their antibodies fade faster than those who tested positive for the virus and also had telltale symptoms.
The study, while small and with limitations, provides a better understanding of a topic that baffles scientists examining this new coronavirus, SARS-CoV-2. Most people who have recovered from COVID-19 develop antibodies, but the extent and duration of that protection remain unknown.
Researchers from Chongqing University of Medicine in China compared the immune responses of 37 asymptomatic people diagnosed with COVID-19 with 37 symptomatic patients in the Wanzhou district of China. Forty percent turned negative for antibodies early in their recovery, compared to only 13% of people who developed symptoms.
Asymptomatic patients also reported lower levels of cytokines, or small proteins released by different cells in the body in response to infection. These proteins, when not controlled, can cause hyperinflammation.
The data suggests that asymptomatic people had a weaker immune response to the virus, echoing the concerns of NIAID Director Anthony Fauci about protecting different antibodies.
“This is not a uniformly robust antibody response, which may be one reason why, when looking at the history of common coronaviruses that cause the common cold, reports in the literature indicate that the durability of immunity that protects is from 3 to 6 months to almost always less than a year, “Fauci said in an interview with JAMA editor-in-chief Howard Bauchner.
The study leaves as many questions as answers. For example, scientists don’t yet know exactly what these declining antibody levels mean, and the lower levels don’t necessarily imply that people who have already recovered from COVID-19 will be vulnerable to reinfection in a few months.
However, the study authors said their results warn against “immunity passports,” or the idea that people who have recovered from an infection should be given some kind of special status so they can travel or return. to work because in theory they are totally immune to reinfection. .
Previous studies on SARS and MERS, two related coronaviruses that have caused previous outbreaks in people, have found that the antibodies last for at least a year. In comparison, this study suggests that antibody levels for the new virus, SARS-CoV-2, may drop much more rapidly.
“Since antibodies are likely a component of COVID-19 protective immunity, this is important to confirm in larger studies,” said Dr. Beth Kirkpatrick, chair of the Department of Microbiology and Molecular Genetics at the University of Vermont.
Antibodies are not the only immune response that the body can generate. Although the immune components that protect against COVID-19 are still unknown, Kirkpatrick said that in some infections, people can still protect themselves even if the antibodies are undetectable low. This is because your immune system, including cells that make antibodies or other parts of the immune system, such as T cells, carries a memory response that can be rapidly stimulated.
Despite finding innate immunity in most COVID-19 patients, public health officials remain concerned about reinfection. There is currently no evidence that people who have recovered from COVID-19 and have antibodies are protected from a second infection, according to the World Health Organization.
“I think you will see that the immune response decreases in these respiratory infections, there is a possibility that it can be reinfected,” said Dr. Robert Garry, professor at the Tulane University School of Medicine.
Garry cautioned, however, that it is too early to know what level of immunity is protective. Scientists will know more as they get closer to developing a coronavirus vaccine, but for now, it would have to provide longer-lasting immunity than a natural infection, he said.
“That’s difficult to do,” said Garry.
Kirkpatrick said that companies may also consider booster vaccines, administered more frequently than might have been expected with SARS or MERS.
The mystery surrounding immunity only reinforces the urgent need for a successful vaccine. Both experts agree that more data is needed to confirm the study findings, but that the mere presence of antibodies may not be enough to immunize the majority of the population.
“Until there is a vaccine, things really cannot relax to the point where people are doing the things they were doing before,” Garry said.
Dr. Alexis Carrington contributed to this report.
What to know about the coronavirus:
Tune in to ABC at 1 pm ET and ABC News Live at 4 pm ET every day of the week for special coverage of the new coronavirus with the entire ABC News team, including the latest news, context, and analysis.
.