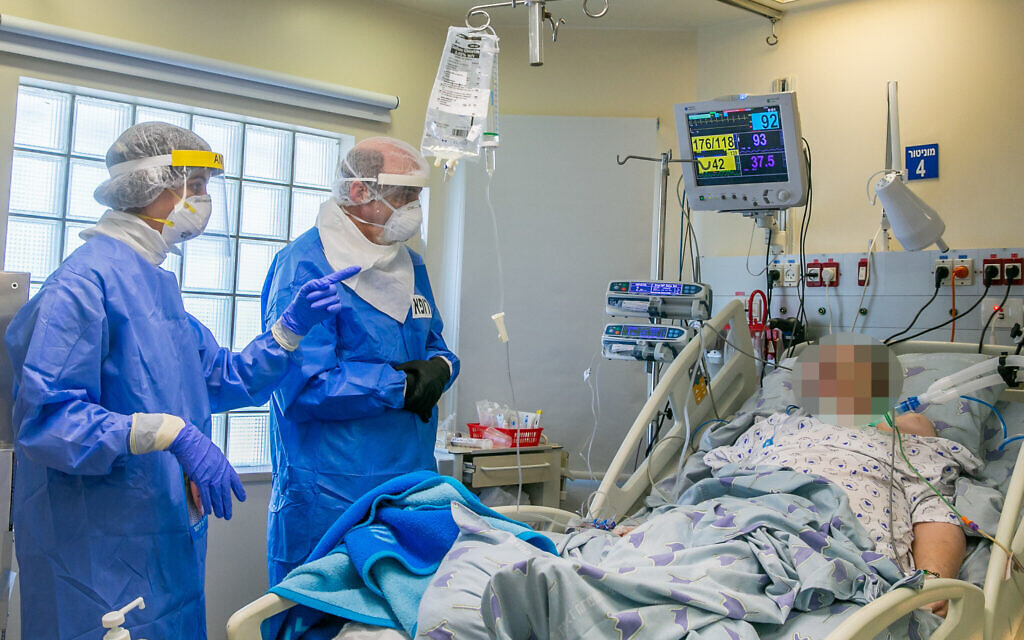
Recovered COVID patients are baffling doctors with complaints of abnormal pain, lungs that simply won’t return to normal, and a variety of disabling psychological problems.
“What we are seeing is very scary,” Gabriel Izbicki, from Jerusalem’s Shaare Zedek Medical Center, told The Times of Israel. “More than half of the patients, weeks after the negative test, are still symptomatic.”
Izbicki is working on a study involving follow-up with patients who were in coronavirus hospitals or hotels, looking at the aftermath of the virus and trying to understand why patients continue to suffer long after being confirmed negative. “There is very little research into the medium-term effect of coronavirus,” she said, adding that there is a great need to guide clinicians.
Get The Times of Israel’s Daily Edition by email and never miss our top stories.
At Bnei Brak, in Israel’s first community clinic, doctors have seen an increase in recent days in patients with pain that seems to come from nowhere.
“It may appear in the arms, legs, or other places where the virus does not have a direct impact, and if you ask about the level of pain on a scale of 1 to 10, it may be 10, with people saying they cannot sleep.” said Eran Schenker, director of the one-month clinic at Bnei Brak, run by Maccabi Healthcare Services. “It’s something that we started to see a lot more in the last week.”

Man coughing (iStock)
‘Broken’ by the virus
A patient at the clinic spoke to The Times of Israel, on the condition that her name not be published. She was diagnosed in March and tested negative a month ago. But the woman, a Bnei Brak resident in her 40s, still has severe fatigue and anxiety, and can only walk for a few minutes at a time.
Her husband, who also contracted a coronavirus in March and tested negative last month, now “feels it is broken,” she said. “It’s actually worse than it was when he was hospitalized.”
Her husband, 55, had some health problems before contracting coronavirus in March, but was active “from morning to night”, with a lot of energy. He is now extremely lethargic, can barely walk, and has heart problems, he said.
This was a particular shock to the family, as during his initial hospitalization in March and early April he did not need oxygen and the radiographs showed no damage to the lungs. Then he was hospitalized again in April with pneumonia-like symptoms and declared negative in May. But the man developed significant respiratory pain and problems, and has seen cardiologists, neurology experts, rehabilitation teams, and other professionals at the clinic.
Schenker said this man is “one of the difficult cases, but he is not the worst and we have patients who suffer more.”
He said that with all illnesses, patients may be reeling from long hospitalizations, and the use of ventilators can delay full recovery, but COVID-19 is causing patterns that are generally not seen.
“We are surprised that people are not only suffering from the things we expected, but the things we simply did not know would be relevant,” he told The Times of Israel. “It is not a textbook.”
He emphasized that his patients are not all newly recovered. “Some of them had coronaviruses in March, so they may have recovered for months,” he said.

Gabriel Izbicki, head of the Pulomary Institute at the Shaare Zedek Medical Center in Jerusalem (Shaare Zedek Medical Center)
Izbicki, director of the Shaare Zedek Lung Institute, also emphasized that many of his patients have been declared free of coronavirus. One of the biggest surprises, he said, is that you cannot predict which patients will find the disease difficult to shake and which will not.
“There is no correlation between the severity of the disease during hospitalization and the extent of symptoms afterward,” he said, discussing the preliminary results of his study in recovered patients who were treated at coronavirus hospitals and hotels.
“Within the symptoms we verified, we revealed general weakness among most patients along with shortness of breath, sustained cough, and other complex respiratory and lung problems,” he said, adding that he is also familiar with the strange pains that Schenker discussed
These pains, seen in young and old patients alike, have doctors scratching their heads. Schenker said: “Painkillers block pain but do not alleviate the source, but we do not know how to address the source and you cannot take pain relievers for the rest of your life.”
While the pains are excruciating for some, others describe the pains more as great discomfort: burning, tingling sensations, or simply a hard-to-identify feeling that a limb is not feeling normal.
Patients with these pains usually do not raise red flags during major medical exams. Schenker said: “We check their lungs and hearts and they are free of disease and neurological problems. We do scans and we can’t see anything, but they have this pain, they tell us over and over again. ”

Dan Oyero, Deputy Director of Medicine in Central Israel for Maccabi Healthcare Services (courtesy of Maccabi Healthcare Services)
Dan Oyero, Maccabi’s deputy director of medicine in central Israel, said the general problem facing doctors is the far-reaching change in people’s lives, for which doctors cannot predict an end point.
“The most distressing thing is that people compare how they feel now compared to how they were a few weeks ago before being infected,” he said. “And they say they just can’t do the things they used to do.”
The sense of taste and smell, lost during illness, sometimes does not return. When patients ask if he will return, since doctors have such limited experience of the disease, they cannot give a clear answer. “We just don’t know,” said Oyero.
When doctors can invoke a precedent for other diseases, it can be bad news.
Elderly patients who were severely affected by the coronavirus, even if they had no previous respiratory problems, may find that their lungs are working at half capacity, long after testing negative, Schenker said.

They were Schenker, director of the clinic for recovered COVID patients at Bnei Brak, run by Maccabi Healthcare Services (courtesy of Maccabi Healthcare Services)
“They have two lungs, but they are the equivalent of one, because each lung is working at 50%, and it could be that way for the rest of their lives,” he said. It draws this conclusion from the pattern of lung damage seen in some other diseases, but which normally only affects patients who had previous lung complications.
“The damage was not caused by the virus, but by a process of inflammation that, as we know from other diseases, will not leave the lungs with the ability to exchange oxygen as before,” Schenker said.
Izbicki said that, in his experience, COVID-related lung damage can affect patients of all ages, and said he shares the concern that people don’t regain full lung performance. “We don’t know if the lung function tests will become normal,” he said.
Some patients require physical therapy. Schenker said: “We have seen cases of weight loss that have been so extreme that people have difficulty walking.” Meanwhile, some who are physically able to move simply do not have the energy or motivation to do so.

A recovered coronavirus patient sees a cardiologist at the special clinic in Bnei Brak run by Maccabi Healthcare Services (courtesy of Maccabi Healthcare Services)
Some of these patients are young and usually energetic, Schenker said.
“It is amazing how many people went back to work, they may be educators, lawyers and other professions, but when they sit for an hour they feel anxious, they feel insecure and sometimes people suffer from depression beyond what we expected.”
Oyero said: “The main complaints are actually fatigue, low energy pacts, nothing we can give a name to. Many people say they don’t have the energy they used to. They are more tired. Some say they don’t have the drive to do things. We can’t name the complaints or tell them they have a particular syndrome, but we are trying to help them. “