
To prevent a dangerous new virus from reaching humanity, you can take a page from Chinese warrior king Sun Tzu and think like the enemy.
Imagine that you are a coronavirus, in a way never seen before by humans. Their goal is simple but tremendously ambitious: invade and hijack the cells of a new host and multiply it for as long as it takes to establish its spawn on at least one other new host.
Repeat until there are no humans left to infect.
Since its appearance in Sun Tzu’s homeland, the coronavirus known to scientists as SARS-CoV-2 has carried out its task with vigor and success. It has easily jumped across national borders, infecting more than 9 million people worldwide and killing at least 470,000 in approximately seven months. The roughly 7.7 billion people who have evaded the infection so far appear to be directly in their sights.
But humanity has some tricks of its own.
Newsletter
Get our free newsletter Coronavirus Today
Sign up to receive the latest news, best stories and what they mean to you, plus answers to your questions.
Occasionally you may receive promotional content from the Los Angeles Times.
In attacks and outbursts, public health officials have brought their citizens together to avoid the kinds of meetings that provide a virus rich in opportunities to spread. Scientists have examined the coronavirus genome to discover secrets about its origin, how it has evolved, and what it will take to thwart it.
Now it’s a race to see which side wins the lead.
Viruses are not as smart as humans, but they are much more patient, said Harvard University epidemiologist William Hanage. And the history of this virus does not bode well for a strategy of ignoring it in the hope that it will burn itself, he added.
“That would be waiting for the virus to help us,” said Hanage. “That is not a good idea.“
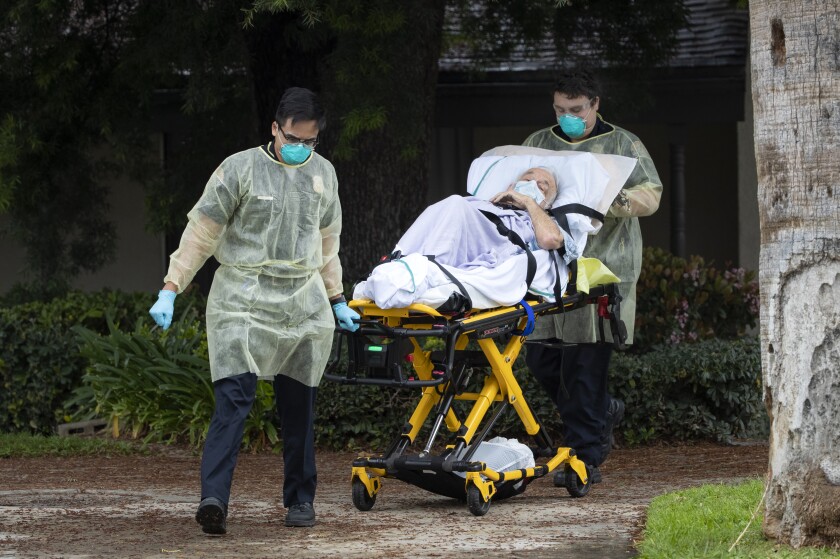
Bernie Erwig, 84, leaves a Riverside nursing home after a test showed she had COVID-19.
(Gina Ferazzi / Los Angeles Times)
Survival imperatives make a successful virus an unpredictable host. cruel to some, kinder to others, and capable of developing new strategies as their group of potential targets grows thinner.
“There is no reward for making a virus lineage easy for its host,” said Frederick M. Cohan, an evolutionary biologist at Wesleyan University.
You shouldn’t kill him right away, as many early forms of the Ebola virus did to his victims. Such outbreaks are bound to fail.
But a successful virus is fine if you leave your victim with an exhausted shell, Cohan said: as long as you’ve managed to make him sick enough to lure others to his side of the bed where they’re exposed to his body fluids or respiratory drops, he’ll live. infect another victim.
You don’t have to be selective about your victims, at least initially. It can save the young and healthy and go after the weak and sick first, as the coronavirus appears to be doing.
But experts believe that a virus that stands the test of time will decrease as its potential hosts decrease and public health precautions are taken.
To continue to spread in such circumstances, a virus must leave many of its victims in good shape to move. It could attack younger hosts, who may not get sick as much but will be better propagators. It could be transmitted by people who don’t even realize they are infected. The coronavirus has done all of this to great effect.
Many viruses have an inherently uphill battle to escalate: as they move through a population, the victims they infect will either die or recover. And those who recover will generally emerge with some immunity.
So after its initial break through a target-rich environment, a new virus discovers that its potential victims have dwindled. People vulnerable to infection are no longer so close. That’s a problem for a respiratory virus like SARS-CoV-2 that can only spread if potential hosts clump together. (Many other viruses spread in water or in the bellies of mosquitoes, fleas, and birds, so social distancing does not counteract them as well.)
An overly aggressive virus can become a victim of its own success, infecting so many people so quickly that it creates what epidemiologists call “collective immunity.” In that scenario, the remaining uninfected targets are too far apart for the pathogen to continue to spread.
Of the seven coronaviruses known to make humans sick, at least four have found a way to circumvent the herd’s immunity and sustain themselves over the long term. These viruses, all of which cause variations in the common cold, leave most of their victims with decreased immunity in just over a year. The group of people who are likely to become hosts is continually renewed as the immune defenses of infected people “forget” the virus that has made them sick earlier.
No one knows if the coronavirus that causes COVID-19 shares that trait. But a large number of studies suggest that, in many of those infected, immunity is weak or transient.
As a matter of evolutionary biology, there is another way to maintain an inexhaustible supply of potential hosts: if a virus can mutate quickly enough, and in specific ways, it can bypass recognition by an immune system that has encountered it before.
The new coronavirus constantly mutates because its genetic instructions are encoded in RNA. Compared to a DNA virus like the one that causes measles, an RNA virus is simpler and less likely to correct the errors that occur each time it replicates.
Most mutations are small nucleotide substitutions that have no effect on the behavior of the virus. But over time, those accumulated errors can change how it looks to an immune system, or how it interacts with its environment or its hosts. And from time to time, a mutation (or a series of them) gives the virus a sudden advantage.

Red Cross members remove patients from a home during the 1918 flu pandemic. By the time the third and final wave ended, an estimated one-third of the world’s population had been infected.
(St. Louis Post-Dispatch)
The 1918 flu pandemic took off after a casual mutation turbocharged its reproductive machinery. The patients became ill more quickly, and with their immune systems fully mobilized, they expelled more viruses when they coughed and sneezed, infecting more people around them.
Scientists have observed how the genetic makeup of the new coronavirus changes, leading some to claim that more virulent and transmissible strains circulate. Those claims have been fiercely debated. But SARS-CoV-2’s ability to shape-shift is what transformed it from a virus that thrived in bats and possibly pangolins into one capable of infecting humans.
Additional mutations could bring new challenges for humans, or new opportunities. If we are lucky, a mutation could make the virus less infectious or less deadly.
But humans have also seized on some tricks to counter viral strategies like these.
Long before our ancestors understood that germs spread disease, they realized that creating distance between people caused fewer people to get sick. During an outbreak, those with means fled the cities for their homes in the country. Those who stayed avoided the market. Public shows were canceled. It was the beginning of the public health strategy that we now call social distancing.
The coronavirus requires people to push close to each other and touch common surfaces to spread from person to person. Social distancing alters the environment to mimic the effects of collective immunity.
The other way to deny a virus to new hosts is to put more people in the “recovered category,” a state that now has more than 4.6 million people.
You do this by letting the pandemic run its course, assuming the immunity will last. Or you can make a vaccine.
Allowing the coronavirus to get away with humanity would be a disaster on a scale between disastrous and unimaginable: Harvard epidemiologist Marc Lipsitch has estimated that with minimal human intervention, SARS-CoV-2 could plausibly infect 20% to 60% of all adults. – Between 1.5 billion and 4.5 billion people. Even if it ends up being no more deadly than seasonal flu, a highly optimistic assumption, between 1.5 million and 4.5 million would die.
A widely deployed vaccine could provide collective immunity, stopping the virus and causing far fewer deaths. But that will take time. Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, has said that parallel efforts to design, test, and produce many vaccines will likely produce at least one by the end of the year.
Until then, this cunning enemy has time on his side and some proven tricks to hold on.
While the coronavirus may not touch everyone on the planet, it appears to have gained the foothold it needs to keep trying, said Columbia University virologist Angela Rasmussen. Like many flu viruses, it could mutate enough from year to year to appear new to our immune system every time it appears. It could also change in ways that make it more like the other four coronaviruses that have infected humans for eons: killing few and making most people sick enough to pass it on.
From a virus standpoint, the definition of success is “becoming the common cold,” said Cohan. Along with many microbiologists, he suspects that this virus has what it takes to go far. Humans could be smarter than a good vaccine, although the immunity it offers may be only temporary. And many who are not afraid of contracting the virus will probably skip it anyway.
He hopes his suspicions are wrong. But a career in studying disease-causing microbes has been punishing, he said.
“We are not smart enough to know what they are going to do,” said Cohan. “And if we think we know, they will simply surprise us.”